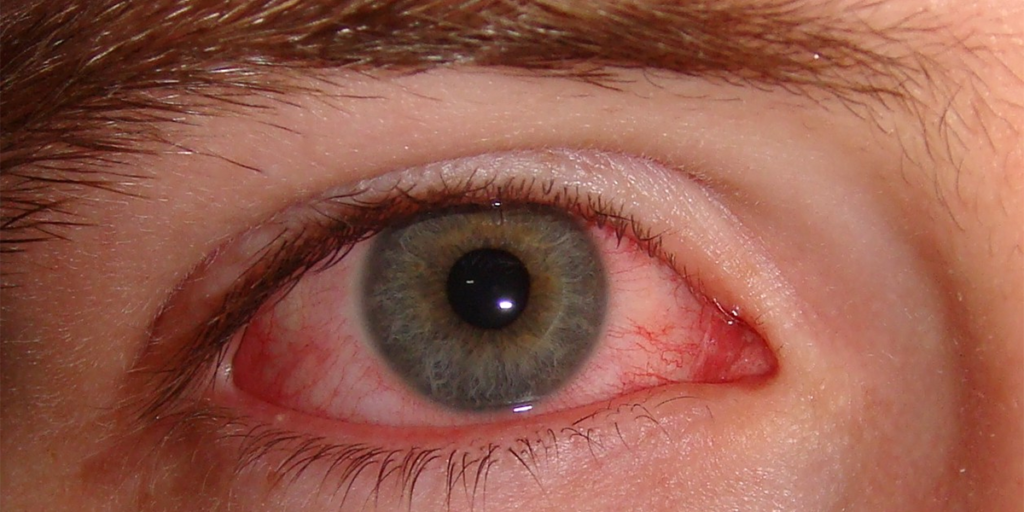
If you’ve ever dealt with medical billing or documentation, you know just how tricky ICD-10 codes can be. On paper, they’re just alphanumeric strings meant to capture a diagnosis. In reality? They’re the key to accurate documentation, clean claims, and making sure patients get the right care without administrative headaches. And when it comes to eye irritation and redness—symptoms that show up constantly in clinics, ERs, and even primary care—choosing the right ICD-10 code can feel like a confusing task.
Let’s understand how ICD-10 classification works for eye irritation and redness, why it matters, and how to apply it correctly.
Why ICD-10 Coding for Eye Symptoms Matters
Eye irritation and redness might seem minor compared to life-threatening conditions, but coding them correctly is crucial for a few reasons:
- Clinical accuracy – A code isn’t just for billing; it tells the clinical story. Is redness allergic? Infectious? Due to trauma? Those distinctions matter in treatment.
- Insurance reimbursement – Payers won’t process vague or incorrect codes. If you simply throw in “eye disorder NOS,” you risk denials or delays.
- Public health data – Accurate coding contributes to research and data collection. Trends in allergic conjunctivitis or infections? They’re tracked through ICD-10.
- Continuity of care – Future providers rely on the coded diagnosis in the chart. If you miss the nuance, it can affect downstream care.
In other words: coding isn’t busywork. It’s the backbone of documentation.
What is the ICD-10 coding system?
ICD-10 (International Classification of Diseases, 10th Revision) is the coding system used worldwide to classify diseases, symptoms, and health conditions. In the U.S., we use ICD-10-CM (Clinical Modification), which adds more specificity.
Each code typically has:
- Category (first 3 characters) – the general condition (e.g., H10 for conjunctivitis).
- Etiology/Details (next 1–3 characters) – the cause or type (e.g., H10.1 for allergic conjunctivitis).
- Laterality (last character, if applicable) – right eye, left eye, or both.
ICD-10’s structure makes it both powerful and irritating as it requires greater specificity.
Common ICD-10 Codes for Eye Irritation and Redness
You can’t simply label a patient’s red, watery, or itchy eyes as “eye irritation” and be done with them. Let’s examine the main ICD-10 codes that are relevant.
Conjunctivitis (H10 category)
Conjunctivitis is one of the most common causes of eye redness. ICD-10 breaks it down by type:
- H10.0 – Mucopurulent conjunctivitis
- H10.1 – Acute atopic conjunctivitis
- H10.2 – Other acute conjunctivitis
- H10.3 – Acute conjunctivitis, unspecified
- H10.4 – Chronic conjunctivitis
- H10.45X – Vernal conjunctivitis (with laterality)
- H10.5 – Blepharoconjunctivitis
- H10.9 – Conjunctivitis, unspecified
Remember that if you’re not sure of the cause, it’s safer to go with “unspecified conjunctivitis” rather than coding something you can’t prove.
Keratitis and Corneal Disorders (H16–H18)
If redness is linked to corneal inflammation, these codes apply:
- H16.0 – Corneal ulcer
- H16.1 – Other superficial keratitis without conjunctivitis
- H16.2 – Keratoconjunctivitis
- H16.3 – Interstitial keratitis
- H16.9 – Keratitis, unspecified
Eye redness due to keratitis often comes with pain, photophobia, or vision changes—so documenting those symptoms helps justify the code.
Dry Eye Syndrome (H04.12)
Dry eye is a huge culprit for irritation and redness, especially in older adults or those with screen-heavy lifestyles.
- H04.121 – Dry eye syndrome, right eye
- H04.122 – Dry eye syndrome, left eye
- H04.123 – Dry eye syndrome, bilateral
- H04.129 – Dry eye syndrome, unspecified eye
Blepharitis (H01.0)
Inflamed eyelids can cause secondary redness. ICD-10 divides it into:
- H01.001–H01.009 – Unspecified blepharitis (with laterality)
- H01.011–H01.019 – Ulcerative blepharitis
- H01.021–H01.029 – Squamous blepharitis
Trauma-Related Redness
Sometimes redness comes from a scratch, foreign body, or injury:
- S05.00XA – Injury of conjunctiva, unspecified eye
- S05.01XA – Injury of conjunctiva, right eye
- S05.02XA – Injury of conjunctiva, left eye
- T15.00XA – Foreign body in eye (unspecified)
Allergic Reactions (H10.1 or T78 series)
If redness is due to allergies:
- H10.10 – Unspecified allergic conjunctivitis
- H10.11 – Seasonal allergic conjunctivitis
- H10.12 – Acute atopic conjunctivitis
- T78.40XA – Allergy, unspecified, initial encounter
General “Red Eye” or Irritation Codes
When there’s no clear diagnosis yet, symptoms can be coded directly:
- H57.89 – Other specified disorders of eye and adnexa
- H57.8 – Other specified symptoms and signs involving the eye and adnexa
- H57.9 – Unspecified disorder of eye and adnexa
These are catch-all codes. Use them sparingly, only if you truly can’t define the condition.
How Laterality Changes Everything
One detail coders often miss? Laterality. Many ICD-10 eye codes require you to specify which eye is affected:
- 1 = Right eye
- 2 = Left eye
- 3 = Bilateral
- 9 = Unspecified
For example:
- H10.021 – Acute follicular conjunctivitis, right eye
- H10.022 – Acute follicular conjunctivitis, left eye
- H10.023 – Acute follicular conjunctivitis, bilateral
If you skip laterality, your claim could bounce back. Always check if the code requires it.
Documentation Tips for Providers
If you’re a provider, you might think coding is the biller’s problem. But remember that bad documentation means bad coding.
Here are some tips to make everyone’s life easier:
- Note laterality (right, left, both eyes).
- Document duration (acute vs chronic).
- Identify the cause if known (allergy, trauma, infection).
- Mention associated symptoms (itching, discharge, photophobia).
The more detail you provide, the easier it is for coders to choose the right ICD-10 code—and the less likely you’ll face claim denials.
Common Mistakes in Coding Eye Redness
- Using unspecified codes too often – It’s tempting, but it weakens documentation.
- Forgetting laterality – One of the most frequent reasons for denials.
- Confusing symptoms with diagnoses – If you know it’s conjunctivitis, don’t just code “red eye.”
- Not updating from ICD-9 habits – Some providers still fall back on outdated coding shortcuts.
The Bigger Picture: ICD-10 and Ophthalmology
Eye irritation and redness are just the tip of the iceberg. ICD-10 has thousands of eye-related codes covering everything from cataracts to retinal detachment. For ophthalmologists and optometrists, knowing these codes isn’t optional—it’s part of running a smooth practice.
And once you start thinking in ICD-10 “logic” like cause, type, laterality—it gets easier to navigate.
The Role of Coders and Billers
Coders aren’t just translators. They’re guardians of accuracy. A skilled coder doesn’t just pick a code; they make sure the documentation supports it, the payer will accept it, and the story of the patient is clear.
For eye conditions, coders often have to chase providers for clarification: “Doctor, was it the right eye or both?” or “Did you confirm it was allergic conjunctivitis, or is it just suspected?”
Strong collaboration between providers and coders is what prevents denials and ensures patients don’t get billed unfairly.
Improving Coding Accuracy and Compliance
One of the biggest challenges in medical coding—especially with something as detail-heavy as ICD-10 for eye conditions—is staying accurate while keeping up with constant updates. That’s where ongoing training makes all the difference. Regular training and education help medical coders stay on top of the latest ICD-10 revisions, payer-specific rules, and documentation standards. It’s not just about passing audits; it’s about making sure the coding truly reflects the patient’s clinical reality.
Another game-changer is utilizing Electronic Health Records (EHRs). When EHRs are integrated with coding software, they do more than just store patient data—they actively support coders and providers with prompts, alerts, and built-in validation tools. This streamlines the entire process, cuts down on human error, and improves compliance with industry regulations. At the end of the day, combining skilled human judgment with smart technology is the best way to keep coding accurate, efficient, and audit-proof.
Final Thought
Eye irritation and redness are not minor complaints, especially in the coding world; they carry a lot of weight. Whether it’s conjunctivitis, dry eye, blepharitis, or trauma, ICD-10 requires precision. It’s not just about getting paid—it’s about telling the patient’s story, guiding treatment, and contributing to the bigger picture of healthcare data. So next time you’re staring at an eye chart—or, more likely, an electronic medical record—remember: those little details (laterality, type, duration) are what turn a vague “red eye” into a clear, billable, and clinically accurate diagnosis.